For decades, when a person with advanced dementia became rigid, when their limbs slowly curled into painful positions, when every attempt at caregiving became a physical struggle, clinicians and families accepted it as part of the disease, one that was often overshadowed by the cognitive changes.
The stiffness is not specifically documented in medical notes or hospital dashboards. It is managed with repositioning, and ultimately attributed to the brain’s deterioration. No one considered whether it might be something distinct, with its own trajectory, something that might even be treatable. A symptom called paratonia.

A Misunderstood Motor Condition in Advanced Dementia
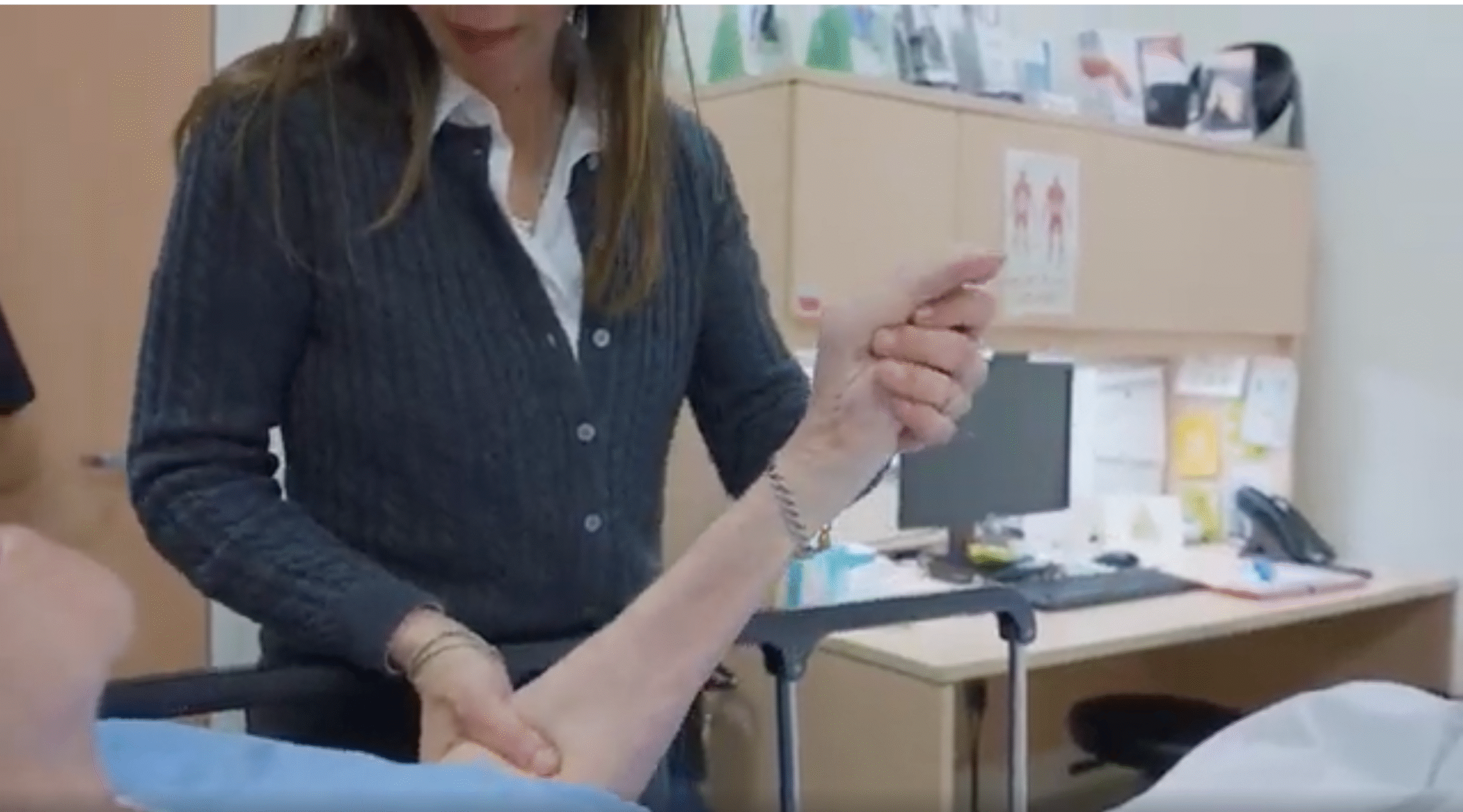
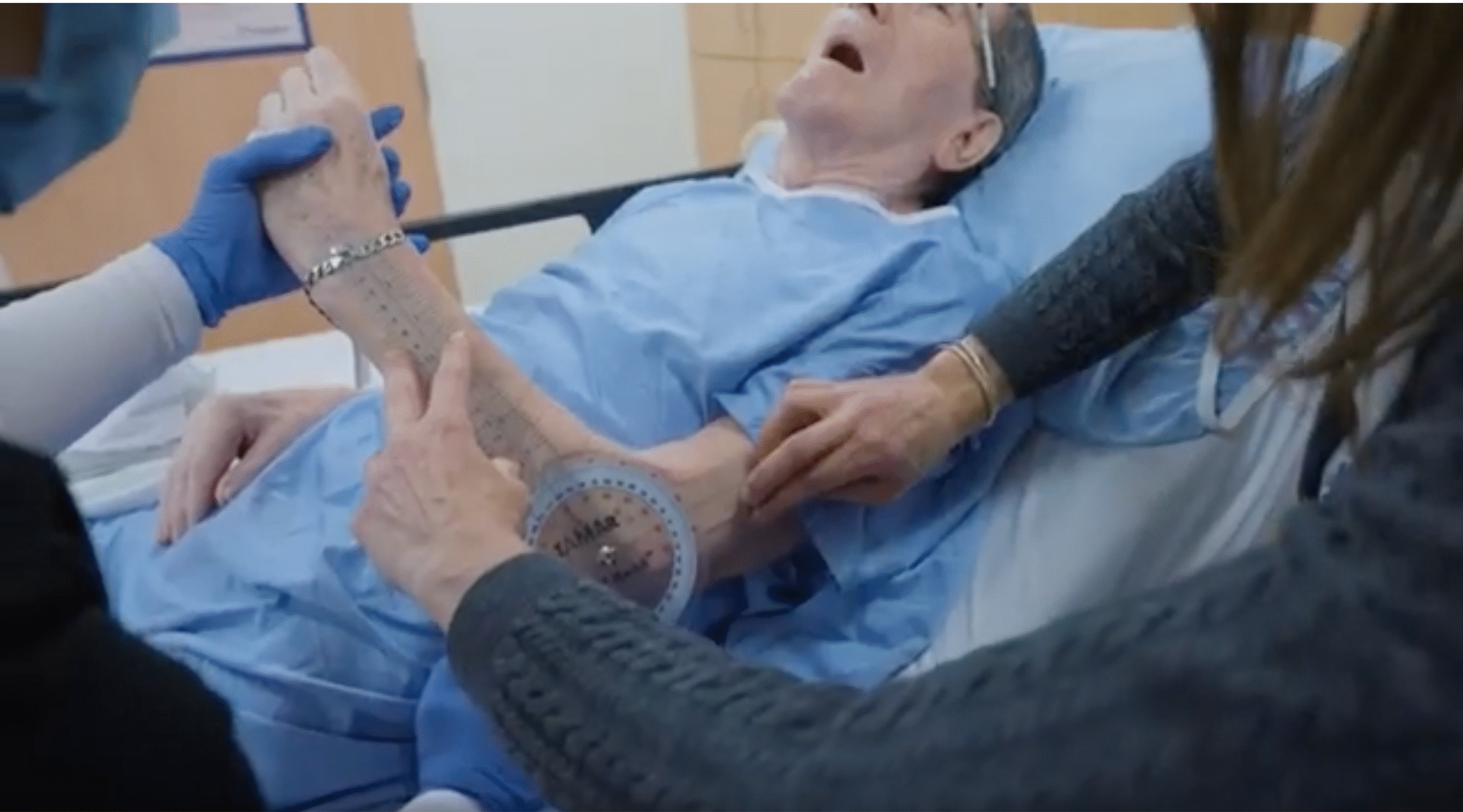
What we now understand as paratonia is a progressive motor condition of dementia. In its early stages, it appears as resistance to care: when a caregiver moves a patient’s limb, the muscles involuntarily resist. As dementia advances, so does paratonia, affecting approximately 10% in the early stages of dementia and increasing to affect nearly everyone with advanced dementia. Over time, limbs become locked into fixed, painful postures.
Because this resistance can appear intentional, it is often mislabeled as “resistant behaviour.” Patients may be inappropriately managed with sedatives or antipsychotics, interventions that may not be appropriate for a body responding to a reflex it cannot control. Without recognition, skin breaks down, pressure injuries form, and routine care can result in fractures. When hands are clenched into fists, a daughter cannot hold her father’s hand. When the body is contorted, a spouse cannot provide a simple embrace without causing distress.
When people witnessed suffering, it was perceived as inevitable, an expected and painful part of the dementia experience. As it turns out, what we were seeing was a potentially treatable condition hiding in plain sight.
The Innovation: Seeing What Was Always There
Progressive muscle changes in dementia were commonly thought of as inevitable, however Dr. Galit Kleiner, a movement disorder neurologist at Baycrest, challenged that assumption. She recognized that the progressive muscle changes in dementia patients represented a distinct motor condition with a name. Where others saw inevitable decline to be managed with pain medication and behavioural interventions, she saw paratonia, an underlying movement disorder that deserved consideration in its own right.
For too long, clinical care has focused on managing the symptoms of paratonia, the pain and the perceived resistance, while missing the opportunity to address the underlying condition itself. Paratonia description exists in scientific literature but has been profoundly neglected in clinical practice. Most healthcare providers have never heard the term. Most families have no idea that the physical resistance they are witnessing every day has a name. The first step toward helping people experiencing paratonia-induced muscle stiffness, is ensuring the condition is recognized: it is not a behavioural problem, but a specific motor condition deserving the same attention we give to movement disorders in any other population.
Over the past decade, Dr. Galit Kleiner has cared for more than 80 individuals living with paratonia, gaining rare, hands-on insight into a condition that has long been overlooked in dementia care. Her clinical experience has led to some preliminary evidence that an existing therapy, already used to reduce muscle hyperactivity in related neurological conditions, may also help ease the involuntary postures that cause pain and care-interference in paratonia.
This emerging opportunity represents a critical moment. Turning these early signals into reliable, evidence-based treatment will require scientific infrastructure that does not yet exist.

Dr. Galit Kleiner, MD, FRCPC is a Staff Movement Disorders Neurologist at the Pamela and Paul Austin Centre for Neurology and Behavioral Supports at Baycrest Hospital, and an Assistant Professor of Neurology at the Department of Medicine, Division of Neurology at the University of Toronto
Building the Research Infrastructure Needed to Advance Paratonia Care
This is the mission of the Paratonia Scientific Development Platform at Baycrest: to create the screening instruments, staging systems, and clinical outcome assessment measures needed to advance this entirely new field. The Paratonia Burden Scale, being designed in accordance with regulatory guidance, will aim to capture the caregiver voice and represent the needs of patients, caregivers, and the health system. This foundational work could enable rigorous trials to one day establish what is safe and effective for reducing the burden of paratonia-induced muscle postures.
Turning Research into Global Solutions for Paratonia
Baycrest is pioneering a grassroots mission that extends far beyond the walls of our campus. We have assembled a vast network of collaborators spanning researchers, clinicians, methodologists, and lay organizations united by the shared purpose of advancing care for people with advanced dementia. Global experts in dementia care, research methodologists, palliative care, and allied health are working hand in hand with dementia representative organizations and advocacy groups. What unites this diverse coalition is a shared commitment to rigorous science and a determination to ease the movement disorder symptoms of dementia and to move the needle for a population medicine has historically overlooked.
The Apotex Centre, Jewish Home for the Aged, Baycrest’s long term care home, creates a rare opportunity to study paratonia in the population most affected. People at the end stage of life are rarely considered research candidates. At Baycrest, we believe the most vulnerable deserve rigorous science directed at reducing their suffering.
Education for Impact at a Global Scale
Education that can scale globally is central to this mission. Dr. Kleiner is developing practical teaching materials to help point-of-care staff, nurses, physicians, and allied health professionals recognize paratonia as a progressive motor condition, not a behavioural choice. These materials will be rigorously tested to ensure they translate knowledge into practice and meaningfully change understanding and care.
The goal is to create educational resources that can be integrated into health systems worldwide, used to onboard point-of-care staff, and shared through dementia representative organizations to reach caregivers and families. When healthcare providers understand what they are seeing, they can choose appropriate approaches and avoid harmful ones. Every person trained to recognize paratonia can deliver more compassionate care today, while helping build the evidence base for treatments of tomorrow.
Rejecting Therapeutic Nihilism
There is a pervasive belief that nothing can be done for people with advanced dementia. This therapeutic nihilism leads us to accept suffering as an unavoidable part of a dementia diagnosis. At Baycrest, we reject this assumption.
Founded in 1918, Baycrest has grown into a globally recognized leader in brain health and aging, with a vision to create a world where every older person lives with purpose, fulfilment, and dignity. We are committed to supporting people throughout their entire health continuum, including at the end of life. That mission means refusing to accept suffering as unavoidable and striving to ease every symptom we can at every phase of life.
The Impact of Research and Education on Paratonia
Building a global research and education platform for paratonia could transform care for people with advanced dementia worldwide. For patients, it means an end to being mislabeled and the possibility of appropriate care to ease suffering. For families, it means understanding what is happening and having the confidence in their providers that appropriate solutions are being pursued. For healthcare providers, it means having tools to respond appropriately. For health systems, it means opportunities to reduce the cascade of complications, hospitalizations, and costs that arise from unrecognized paratonia.
Baycrest is exceptionally suited to lead this transformation. As one of the world’s top academic health sciences centres in aging and brain health, the #1 most research-intensive hospital focusing on neuroscience and aging in Canada, we are uniquely positioned to combine over a century of compassionate care with rigorous science through the Rotman Research Institute, the Centre for Aging and Brain Health Innovation and a network as the hub of the Canadian Consortium on Neurodegeneration in Aging (CCNA).
This specialized expertise includes over 15 years of medical experience in identifying and caring for people with paratonia-induced muscle postures, supported by a unique 10-year patient database capturing the lived experience of paratonia. No other organization brings together this combination of clinical depth, research infrastructure, and global collaboration under one roof.
Be a Part of the Paratonia Solution
Your support could help build the research and education platform that makes paratonia a recognized, studied, and addressable condition worldwide. It will fund screening tools, staging systems, and outcome measures. It will enable us to create rigorously tested educational materials that can scale across health systems globally. It will empower a coalition of researchers, clinicians, and advocates united by common purpose.
This is a grassroots mission to ensure that every person, at every stage of life, receives dignity, comfort, and hope. Together, we can change how the world cares for people with advanced dementia.
Frequently Asked Questions About Paratonia
What is paratonia?
Paratonia is a progressive motor condition associated with dementia that causes involuntary muscle resistance during movement. When a caregiver moves a limb, the muscles automatically resist, even though the person is not consciously opposing care.
Is paratonia a behavioral symptom of dementia?
No. Paratonia is not a behavior or choice. It is a neurological motor reflex caused by brain changes in dementia. Mislabeling it as “resistant behavior” can lead to inappropriate treatments and increased harm.
How common is paratonia in dementia?
Paratonia affects about 10% of people in early dementia and becomes increasingly common as dementia progresses. In advanced dementia, nearly everyone experiences some degree of paratonia.
What are the main symptoms of paratonia?
Symptoms include involuntary resistance to movement, progressive muscle stiffness, clenched fists, limbs locked into painful positions, and increasing difficulty with routine care such as dressing, bathing, or repositioning.
Why is paratonia often missed or misunderstood?
Paratonia is rarely taught in clinical training and is not routinely documented in medical records. Because the resistance looks intentional, it is often mistaken for agitation or non-compliance rather than a motor condition.
Can paratonia cause pain or injury?
Yes. Untreated paratonia can lead to chronic pain, pressure injuries, skin breakdown, fractures, and infections. Routine caregiving can unintentionally cause harm when the condition is not recognized.
Is there any evidence of a treatment that can ease the pain of paratonia?
There is currently no approved treatment for paratonia, but at Baycrest there is clinical experience leading to preliminary evidence that an existing therapy used in related neurological conditions may also ease the involuntary postures related to paratonia. Rigorous research is needed to determine what is safe and effective.
What is Baycrest doing to advance paratonia care
Baycrest is developing the Paratonia Scientific Development Platform, a comprehensive initiative that extends well beyond traditional research. The platform encompasses developing educational materials for clinicians and caregivers, creating screening tools to identify paratonia in nursing home populations, building a validated outcome measure (the Paratonia Burden Scale) to support future clinical trials, and surveying caregivers to understand what matters most to families living with this condition. Baycrest is also leading efforts to establish clinical guidelines for standardized care practices, advocating for health policy changes to improve access to care, and building an international coalition of advocates, scientists, and clinicians committed to making paratonia a recognized and treatable condition.
Why study paratonia in advanced dementia?
People with advanced dementia are most affected by paratonia yet are often excluded from research. Studying paratonia in this population is important to reduce suffering and improve end-of-life care.
How does recognizing paratonia improve care?
Recognition shifts care toward safer, more compassionate approaches, reduces complications such as permanent joint contractures that can develop when paratonia goes unidentified, helps families understand what is happening, and gives healthcare providers appropriate tools to respond. Early identification also enables timely intervention before irreversible deformities become established, helps avoid potentially harmful treatments based on misdiagnosis, and allows eligible individuals to be identified as candidates for future clinical trials investigating new treatment approaches.
Why is education important for paratonia care?
Paratonia education is largely absent from medical, nursing, and allied health training curricula, which means most healthcare providers have never learned to identify it. Without education, paratonia is frequently misinterpreted as intentional resistance to care, leading to forceful handling that can cause pain, fractures, and skin breakdown, or misdiagnosed, leading to inappropriate treatment approaches.
Education helps clinicians and caregivers recognize paratonia as a distinct neurological condition with its own assessment and management considerations. It also challenges the deeply entrenched belief that progressive stiffening and pain in advanced dementia are inevitable and untreatable, empowering providers and families to seek appropriate care rather than accept suffering as an expected part of the disease.How can I support paratonia research?
Supporting Baycrest funds research tools, clinical assessments, and education programs that aim to make paratonia a recognized, studied, and addressable condition worldwide.
Related Articles: Brain Matters, Research, Innovation, Care, Education